Nail (Subungual) Melanoma: What to Look For, Why It’s Missed, and Why Early Investigation Matters
Melanoma can develop under or around a fingernail or toenail (often called nail unit or subungual melanoma). It is uncommon, but it matters because it is frequently misinterpreted as something benign—a bruise, a fungal nail infection, or a normal pigment streak—and this can delay diagnosis.
What is nail (subungual) melanoma?
Nail melanoma arises from melanocytes within the nail unit, often the nail matrix (the growth area under the cuticle).
It most commonly affects a single nail, particularly the thumb or big toe.
What are the most important warning signs?
- A new or changing dark streak in ONE nail
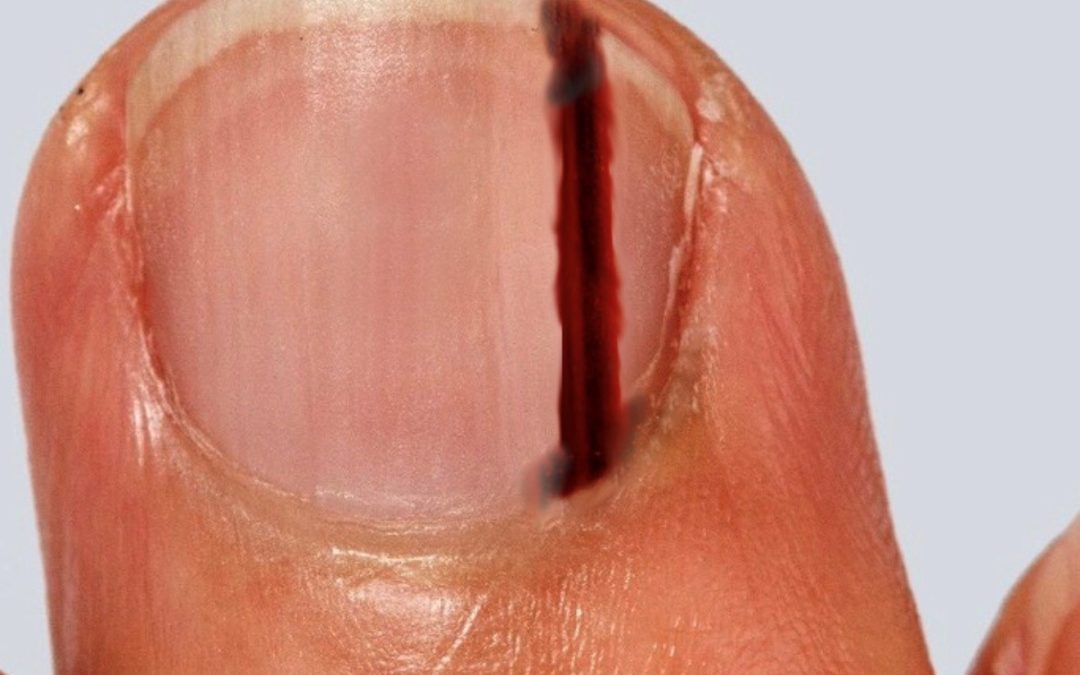
The classic early sign is a brown-to-black vertical band running along the nail (longitudinal melanonychia). What raises concern is not just the presence of a band, but change over time.
Red flags include:
- the band widens (especially at the base near the cuticle)
- the colour becomes darker
- the borders become irregular
- the pigment becomes more obvious or extends further down the nail over weeks to months
- Pigment on the skin around the nail (Hutchinson sign)
A major warning sign is pigment spreading beyond the nail onto the cuticle or surrounding skin (Hutchinson sign). This is an important clue that the pigment may be coming from a malignant process in the nail matrix.
- Nail changes: splitting, distortion, lifting, ulceration, or bleeding
Nail melanoma can also present with nail dystrophy—a nail that becomes misshapen, splits, breaks, lifts, or develops ulceration/bleeding—sometimes with little obvious pigment.
- A “bruise” that doesn’t behave like a bruise
A true bruise under the nail typically moves outward as the nail grows. A persistent dark area that doesn’t grow out, especially without a clear injury history, deserves medical review.
Why is nail melanoma often missed?
Two of the most frequent misdiagnoses are:
- benign pigment streaking (striate/longitudinal melanonychia from non-cancer causes)
- onychomycosis (fungal nail infection)
It can also be mistaken for trauma-related bruising, a nail nevus (mole), inflammation, or a bacterial infection.
People don’t think to check nails.
Public education on melanoma often focuses on sun-exposed skin and moles. Nails—especially toes—are easy to overlook during self-checks.
Confirming the diagnosis usually requires a carefully planned biopsy of the nail unit (often involving the nail matrix), which is more complex than a routine skin biopsy. It is best done by a plastic surgeon.
Why is early investigation so critical?
Early detection is vital because melanoma outcomes are better when diagnosed at an earlier stage, before deeper invasion or spread. For nail melanoma, delays are common because it can look harmless at first.
The most important practical message is: a new or changing pigmented streak in a single nail should be assessed promptly—especially if it is widening, darkening, irregular, or associated with pigment on the surrounding skin or nail distortion.
When should you book an urgent assessment with a plastic surgeon?
Seek prompt medical review if you notice:
- a new dark streak in one nail (thumb or big toe especially)
- a streak that is widening, darkening, or becoming irregular
- pigment appearing on the cuticle/nail fold
- nail splitting, lifting, bleeding, ulcerating, or becoming distorted
- a dark area under the nail with no clear injury or that doesn’t grow out
Recent Comments